Weight loss: What are the differences between Ozempic and Mounjaro?
A plethora of new weight loss drugs are now available, but they are not necessarily the same. Here is a guide to the latest GLP-1 receptor agonists.
New drugs that promote weight loss and treat diabetes have taken the public and the pharmaceutical industry by storm. The latest addition, Mounjaro, has recently joined Ozempic, Wegovy, Victoza, and others in a growing class of drugs called GLP-1 receptor agonists. With about half a dozen drugs available and more in development, many doctors say these drugs are revolutionizing the treatment of obesity, type 2 diabetes, and other metabolic diseases.
But keeping track of the many options can be challenging. Although the new drugs tout similar end results and side effects, doctors say that different drugs may be best suited for different people.

The origins of GLP-1 receptor agonists
The human intestine naturally produces a hormone called GLP-1 in response to food intake. When GLP-1 binds to specific receptors in the body, it triggers a series of mechanisms that regulate blood sugar levels, slow down the movement of food through the digestive system, and act on neurons in the brain—all of which lead to a feeling of fullness that helps people eat less and lose weight.
Natural human GLP-1 breaks down quickly in the body, and its effects are short-lived. In the 1990s, pharmaceutical companies began developing a longer-lasting version to treat diabetes. In 2005, a synthetic version called exenatide—inspired by a more stable compound—was approved by the US Food and Drug Administration (FDA) as the first GLP-1 receptor agonist.
In pharmacology, a receptor agonist mimics another substance, such as a hormone, by binding to its receptor. Scientists have continued to build on the first GLP-1 receptor agonist and develop versions that are more effective and easier to administer. Some even show promising signs for treating other diseases, such as heart disease and alcohol addiction.
Liraglutide and dulaglutide: The oldest generation
Exenatide is rarely used today, and two other drugs called liraglutide and dulaglutide are now the oldest GLP-1 receptor agonists still in widespread use. Both were first approved for the treatment of type 2 diabetes. Liraglutide is sold as the weight loss drug Saxenda and the diabetes drug Victoza, while dulaglutide is sold as Trulicity, which is only approved for diabetes.
Neither liraglutide nor dulaglutide regulate blood sugar or weight as effectively as newer versions, but these older drugs are still good options for people with mild diabetes who are not overweight.
Both liraglutide and dulaglutide must be injected regularly—liraglutide daily and dulaglutide weekly. Their molecular structures differ, but there are really no major differences in their effects on blood sugar control and body weight.
Semaglutide: The dawn of a new era
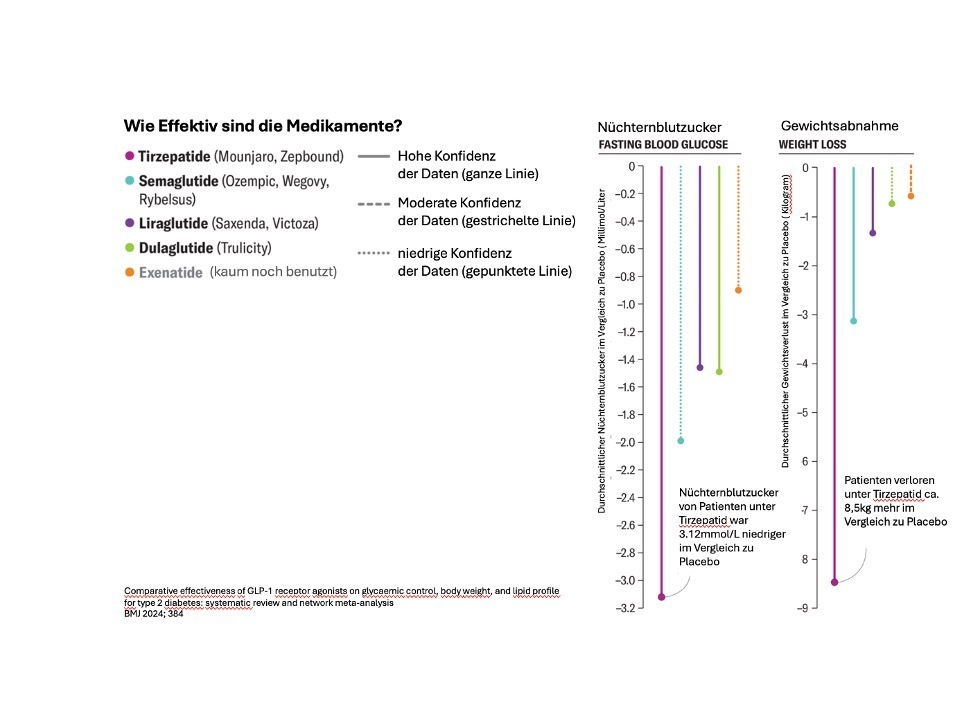
The first generation of GLP-1 receptor agonists led to an average weight loss of less than 10 percent. Newer drugs can help people lose about 15 percent of their body weight.
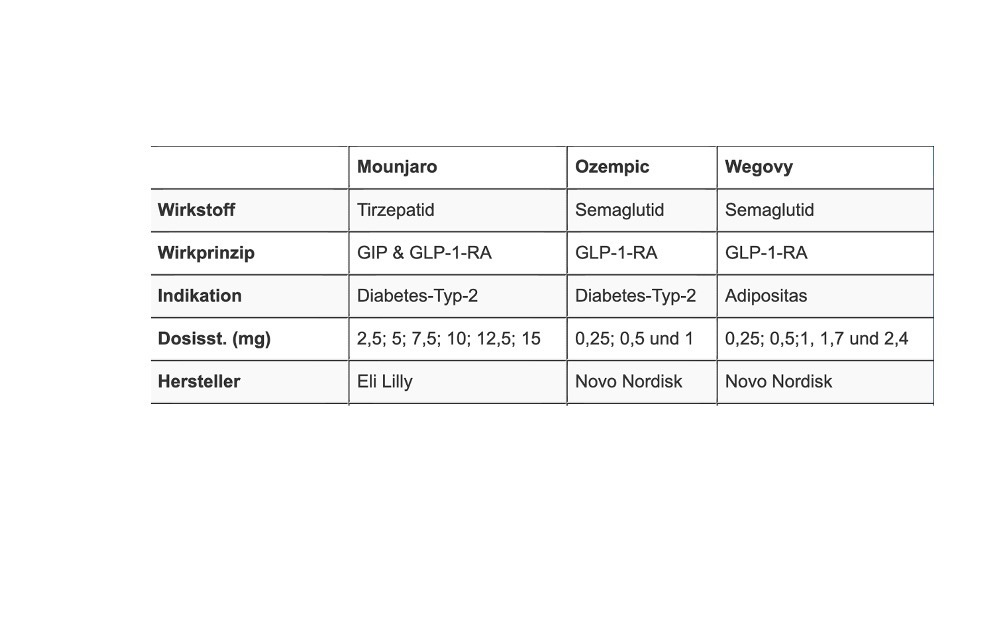
This progress began with FDA approval of a new GLP-1 receptor agonist called semaglutide, known as a weekly injection for the treatment of type 2 diabetes under the brand name Ozempic. The drug was first approved for this purpose in 2017 and later approved as a type 2 diabetes tablet under the name Rybelsus and, more recently, as an injection for the treatment of obesity under the name Wegovy.
Semaglutide showed a "modest but significant advantage" over dulaglutide in controlling diabetes and promoting weight loss. However, it is still unclear which aspects of semaglutide give this molecule this advantage.
Semaglutide is also the first (and so far only) GLP-1 receptor agonist that has been shown to reduce the risk of heart attacks and strokes in people without diabetes.
Tirzepatide: A two-pronged attack
A new player called tirzepatide entered the GLP-1 receptor agonist game in 2022. This drug was first approved for the treatment of type 2 diabetes under the name Mounjaro and, at the end of last year, also for weight loss under the name Zepbound. Tirzepatide is the first agonist to interact with a second receptor, known as glucose-dependent insulinotropic polypeptide (GIP), which affects insulin levels and blood sugar in a similar way to GLP-1.
This dual action likely allows tirzepatide to control blood sugar better than its predecessors. Clinical trials show that the drug can help people lose 20 percent or more of their body mass—more than any previously approved agonist. Researchers continue to explore several hypotheses as to why tirzepatide is so effective at weight loss. The drug's interaction with GIP could underlie its impressive results, or it could activate a different pathway than natural GLP-1 when it binds to the GLP-1 receptor.
Tirzepatide: Not yet proven to protect the cardiovascular system, but promising
Tirzepatide has not yet been shown to reduce the risk of heart attacks or strokes, but studies are currently underway.
Possible uses and side effects
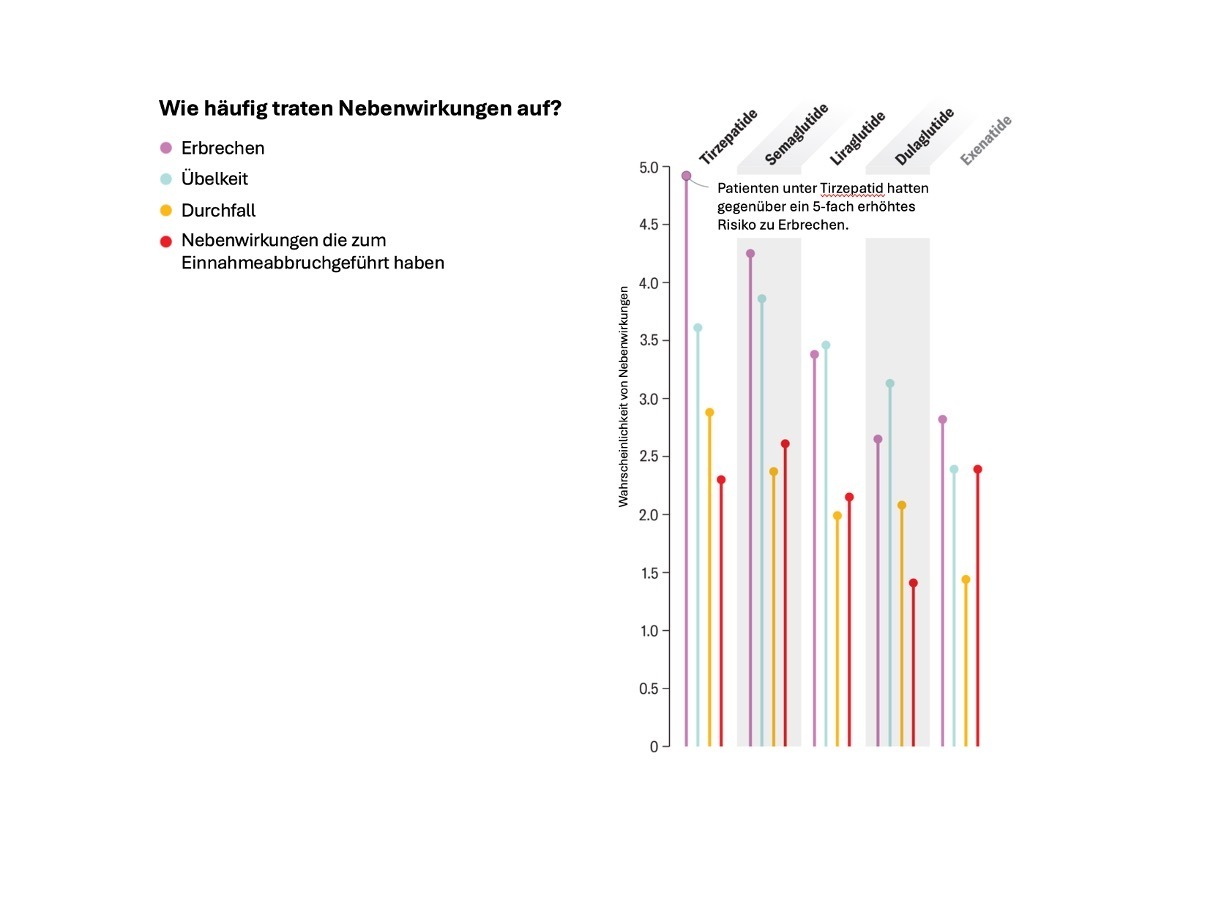
However, the success of tirzepatide could also have disadvantages. There is a trade-off between efficacy and side effects. Initial study data suggest that semaglutide and tirzepatide—which offer greater control over blood sugar and body weight than liraglutide and dulaglutide—may also be associated with a slightly higher chance of unpleasant symptoms (diarrhea, nausea, and vomiting).
The side effects of GLP-1 receptor agonists are usually mild and manageable, but some people cannot tolerate these drugs at all. They should also be used with caution in people with certain other conditions, such as retinal disorders, as these could worsen if blood sugar drops too quickly.
Growing options despite limited availability
Companies are working quickly to develop the next improved generation of GLP-1 receptor agonists. Of the dozens in development, two have particularly high potential to make a difference. The first, called retatrutide, is being developed by the same manufacturer as tirzepatide and would be the first to interact with a third receptor in addition to GLP-1 and GIP. This third target receptor, the glucagon receptor, regulates blood sugar and could also influence food intake and fat storage. The second, CagriSema, combines semaglutide with a synthetic version of a hormone called amylin, which also promotes satiety. Initial tests suggest that both could offer even better blood sugar control and weight loss than current options.
More options could help close gaps in access. High prices have made GLP-1 receptor agonists unaffordable for many people, especially in low-income countries. Insurance companies are more likely to cover the costs when the drugs are used to treat diabetes than for weight loss—a frustration for people without diabetes who seek the benefits of weight loss and would like to avoid costly health complications for themselves and society. Patients thus find themselves in a debate about which conditions are worth treating and which are not. For example, breast reduction surgery is much more readily covered for men than for women; the same applies to horrendously expensive tumor treatments that offer only a few weeks of survival advantage compared to weight-loss drugs such as Wegovy or Mounjaro.
It is difficult to prescribe a less effective drug "when you know there is something better," says Dr. Stefan Schlosser, obesity expert and gastroenterologist in Bern.
Beyond weight loss and diabetes, researchers are also investigating a growing list of conditions that could be treated with GLP-1 agonists. Recent publications suggest that these drugs may dampen overactive immune responses in the brain—a process that could help treat neurodegenerative diseases such as Parkinson's and Alzheimer's.
"I really think the future of this area of medicine is very promising," says Dr. Schlosser.
Wegovy vs. Mounjaro: Key findings
The latest developments in GLP-1 drugs are impressive and have attracted a lot of attention worldwide. However, these drugs should not be considered miracle cures. They are designed to be used in combination with lifestyle changes to achieve sustainable results. The diabetes drug Mounjaro (tirzepatide) has shown remarkable success in weight loss. Current clinical studies suggest that Mounjaro may be more effective than Ozempic. Patients taking Mounjaro achieved an average weight loss of 26.6% within 84 weeks. Mounjaro promotes weight loss by increasing satiety, breaking down fat, and reducing sugar cravings. Side effects are similar to those of Ozempic and include nausea, vomiting, abdominal pain, and constipation. However, Mounjaro may have more side effects than Ozempic, and long-term studies on these side effects are still pending.