What is obstructive defecation syndrome (ODS)?
Obstructive defecation syndrome is a voiding disorder of the rectum (bowel evacuation disorder or defecation disorder) caused by
- a ventral rectocele (internal protrusion of the rectum towards the front) or
- an internal rectal prolapse (a part of the rectum protrudes into itself, also known as internal rectoanal intussusception).
Adequate diagnosis and treatment of voiding dysfunction is a challenge due to the wide range of causes, complex manifestations and differentiated treatment options.
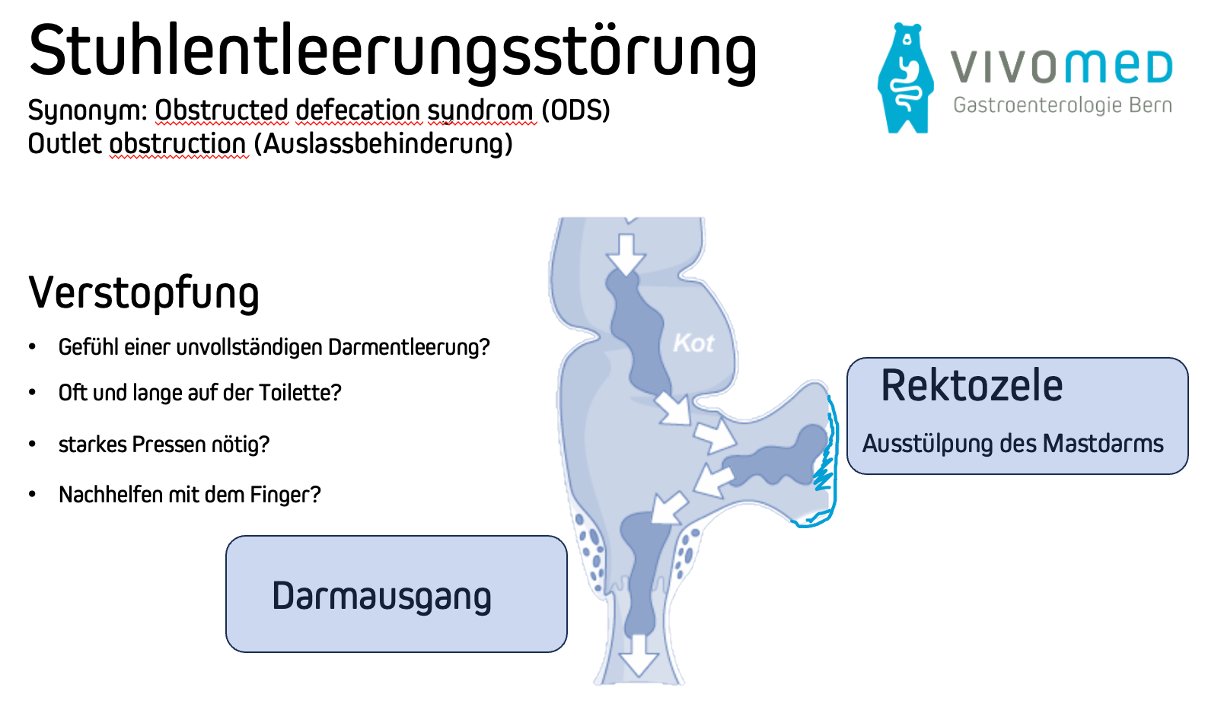
Diagram of defecation disorder
A differentiated diagnosis is important, whereby the following causes must be excluded:
- Primary internal causes of chronic constipation (metabolic, endocrine, neurological-psychiatric, drug-related)Colonic transport disorder (slow transit constipation)Segmental transport disorder (diverticulitis, sigmoidocele)Functional disorders (coordination disorder, pelvic floor dyssynergia, anismus, spasticity)
What symptoms do patients with ODS have?
- Feeling of incomplete evacuationSuccessful, repeated attempts to defecateIntense strainingUse of laxatives and enemasProlonged defecationEvacuation of stool only with the aid of fingersPain and feeling of pressureSmearing stoolDifficulty holding stool voluntarily Bleeding
What changes are detected?
The ventral rectocele is one of the most common changes that can be detected in defecation disorders. Women are usually affected. The ventral rectocele usually occurs in combination with other pelvic floor dysfunctions, so that the cause of the voiding disorder is usually difficult to determine and to pinpoint to a single cause.
What treatment options are available?
The treatment approaches for obstructive defecation syndrome (ODS) can vary depending on the individual causes and symptoms. Here are some common treatment options:
Lifestyle and dietary changes: adjusting dietary habits, promoting fiber and adequate hydration can improve symptoms.
Biofeedback: This is a technique that uses electromyographic (EMG) sensors to measure the activity of the pelvic floor muscles. Through targeted training, the patient can learn to control the muscles more consciously.
Physiotherapy: Specially trained physiotherapists can instruct exercises to strengthen and relax the muscles in the pelvic area.
Drug therapy: In some cases, medication such as laxative preparations or muscle relaxants can be prescribed to support bowel function.
Surgical intervention: In severe cases where conservative measures are not sufficient, a surgical option may be considered. This includes procedures such as sacral nerve stimulation or removal of obstructions in the bowel.
The choice of treatment depends heavily on the exact cause, individual symptoms and the severity of the condition. It is important that an experienced physician performs a comprehensive examination to determine the most appropriate therapy for the individual patient.